Quick Points
The problem
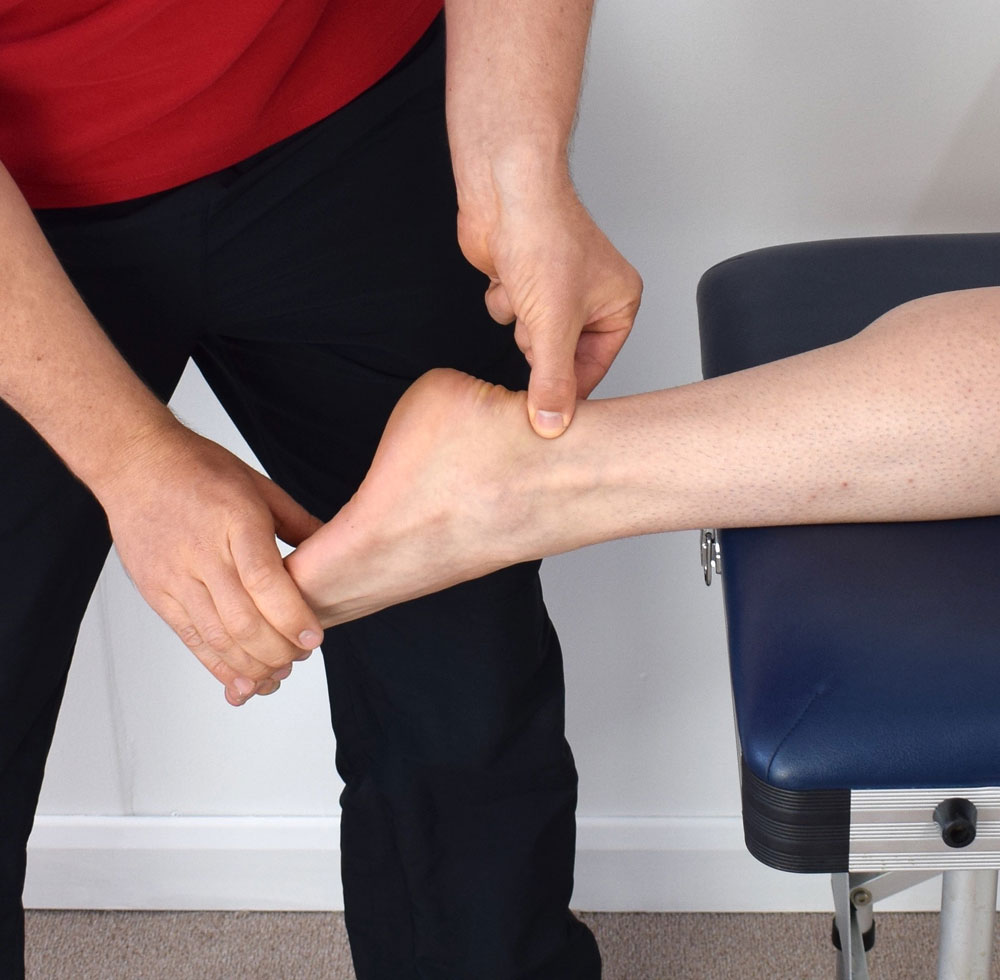
- The Achilles tendon is the large tendon at the back of the ankle that attaches the calf muscles to the heel.
- The attachment of the Achilles tendon allows your heel to come up when walking, running, jumping, or standing on your toes. It also allows the power generated in your calf muscles to be transferred to a push off through your toes during these same activities.
- Achilles tendinopathy often occurs as an overuse injury from activities such as running or jumping that strain the tendon
Hints for self-management
- Decrease the intensity of your exercise routine
- Cross train to decrease stresses through the Achilles tendon
- Ice the area for 20 minutes after exercise, or when you feel pain
- Anti-inflammatory medication may help to manage pain
- Gently stretch the calf muscles
Interesting facts
- The Achilles tendon is the largest tendon in the body.
- Achilles tendinopathies account for about 11% of all running injuries.
- Achilles tendinopathy can either be acute, occurring within a few days after a sudden increase in activity, or chronic, progressing over a period of weeks to months.
Management options
- Braces/taping for support and to unload the tendon
- Eccentric exercises to strengthen the tendon
- Cortisone injections are rarely used around the Achilles tendon but can be beneficial in some specific cases
- Anti-inflammatory creams/patches or medication may be prescribed by your doctor
- Autologous blood injections are currently undergoing trials to determine how helpful they can be
What you can expect/look out for
- Pain above the heel after running or other sports activity
- Increasing pain associated with activities involving prolonged running, jumping, or stair climbing
- Tenderness on palpation, possibly with a small swelling on the Achilles tendon
- Tenderness and stiffness, especially in the morning, that improves with mild activity
Other information
- Help avoid developing future episodes of Achilles tendonitis by increasing running no more than 10% per week
- Eccentric loading exercises have been proven to strengthen and remodel chronically damaged tendons
- Ultrasound imaging can be used to differentially diagnose a tendon injury
- Unloading the tendon in the initial phases will help with pain. These can include taping, heel raises and orthotics
Detailed Information
Achilles Tendinopathy is a degenerative condition characterised by pain and stiffness in the Achilles tendon.
It is different from it cousin Achilles Tendinitis because in tendinopathy there is an absence of an acute inflammatory response and therefore it is often poorly responsive to Non-Steroidal AntiInflammatory (NSAID) medications.
A misconception is that as a tendon degenerates it becomes thinner and more prone to tearing like a cartoon rope but this is an inaccurate image and one that can lead to chronic pain behaviours.
Degenerative tendons look more like old rope which has thickened. Micro tears have occurred but the overall effect is that the tendon is thicker
Thats often why the tendon feels thicker than on the non-affected side and may contain focal nodules.
It’s important to realise that this does not mean that your Achilles is going to snap…far from it, in fact there is no evidence that shows that achilles tendinopathy progresses into tears.
So…thats all well and good….but what to do about it?
Well.. let’s look at it from a microscopic perspective…if we want the tissues to heal and recover we have to cease irritating it. ACTIVITY modification is, therefore, an important step…In other words, REST…take it easy. Even the use of heel raises can offload the tension in the system, this can be especially useful in the more painful early stages.
Kinesiotape (stretchy elastic tape) can be used…and it looks so cool too!! (thats me being sarcastic!). Use it if it creates at least a 50% reduction in symptoms if it doesn’t don’t worry.
Application of ice and ice cube massage has been shown to cause a local vasoconstrictive response which can reduce neovascularisation (or the creation of useless small blood vessels that impede the healing process). It’s worth a try.
Current evidence supports the use of extracorporeal shockwave (ESWT) therapy (a machine that works like a mini jackhammer!) and eccentric exercise. Although the link just posted shows the patient dropping from a normal step, new research indicates there may be additional benefit from having a rolled towel placed underneath the toes to further increase the windlass effect of the foot. There appears to be a benefit in adding loading to the exercise, even if it induces some pain.
Dynamic calf stretching and foam rolling have also been shown to have some beneficial outcomes for some so they are worthwhile adding into management program, but the mainstay of management still needs to be eccentric exercise.
Despite implementing these strategies some people may suffer from persistent or recalcitrant pain. For these it may be worthwhile discussing with their doctor whether glycerin trinitrate (GTN) patches would be a worthwhile addition. The jury is still out as to whether injections should play a role in management with a 2015 Cochrane Review reporting that there was little evidence to suggest injection therapy (including Cortisone and Plasma Rich Protein (PRP) injections) was worthwhile. It seems the key is
- let it settle
- address any biomechanical dysfunction
- load it progressively over time. But the most important thing?….
Be patient and be positive.
Treatment
There are a few key points to consider when rehabilitating your tendinopathy. It is a complicated condition and will often take many months for your pain to settle and return to normal sporting activities pain-free. The majority of this blog will focus on exercise, as this is the most evidence-based treatment for tendinopathy. Before discussing exercise options to improve tendon strength we will touch on a few common treatment options:
- Rest: tendinopathy does not improve with rest as it does not improve the affected tendon’s response to load. Although pain may initially settle, it often returns with a return to activity
- Anti-Inflammatories: these may help reduce pain levels but have no effect on tendon structure, as it is not considered an inflammatory condition.
- Shockwave Therapy: Evidence on shockwave therapy is mixed, mostly due to the type of study conducted. The best evidence is in plantar heel pain (e.g. plantar fasciitis). It does seem to have a good short-term effect on pain and therefore is often a useful adjunct to exercise.
- PRP Injections: Overall, there is poor evidence for any type of injection in tendinopathy. Currently one of the most common options is a PRP injection. PRP injections are derived from spinning a blood sample to separate the platelets that contain growth factors and promote healing. This is then injected into the tendon to stimulate healing. In good quality studies, PRP does not perform better than placebo. In fact, it was removed from the Medicare rebate scheme due to a lack of evidence and the high cost. It, therefore, should only be considered a last resort in stable tendon pain.
Tendons need to be loaded progressively so that they can adapt and develop a tolerance to each individual’s specific activity. In most cases, tendinopathy will not improve without this increase in loading. Although rest does not heal tendons, there is a need to modify some aggravating factors in order to allow the tendon time to adapt to the exercises. Exercise needs to be individualised based on your individual pain, function and goals. Current evidence supports a progressive exercise program that is progressed over months according to each person’s response. These programs can be broken down into 4 key phases:
- Isometric Exercise (pain relief): recent evidence shows long sustained holds for 5×45-60sec may have a pain relieving effect in tendinopathy.
- Strength: once symptoms allow, progressing to specific heavy, slow exercises of 4×6 up to 3x per week allow for muscle growth.
- Power & Speed: reducing weight from phase 2 but increasing speed, up to a maximum of 3 sessions per week.
- Sports Specific: every 2-3 days while continuing strength exercises.
As you can see, tendinopathy is a complicated condition that requires a very clear and multifaceted approach to achieve the best possible outcomes. Unfortunately, there is no shortcut or quick fix to treating tendon pain. Exercise is the best medicine, with everything else being an adjunct to a well planned, personalised and progressive rehabilitation program. It is important to get a review by a therapist confident and experienced in treating tendinopathy as it can often be a debilitating condition that will hang around for months without appropriate treatment.
A final note from a Sports Physician John Orchard who has a special interest in tendons
The body – eventually – does a good job of curing the pain of Achilles tendinopathy itself in the vast majority of patients, probably with the help of the patient being advised or stumbling upon the formula of moderately loading the tendon just enough to strength it but not enough to overload it.